Psoriasis
What is psoriasis?
Psoriasis is a commonly seen chronic and inflammatory skin condition that results in red, thickened, flaky patches of skin covered with silvery scales that may be sore or itchy. It can occur on many different areas of the body, but most commonly seen on the skin of the elbows, knees and scalp. Psoriasis can also affect the nails (nail psoriasis), or the joints that may cause arthritis (psoriatic arthritis).
Although psoriasis can affect people of any age, it is most commonly seen in those aged between 11 and 50. It tends to affect men and women equally. The condition is not infectious, nor is it contagious.
What can cause psoriasis?
The exact cause of psoriasis is not known; however, it is generally accepted that overactivity of the immune system in the skin plays a part in the development of the condition, as well as inherited factors in some cases.
In psoriasis, a type of immune cell known as a T lymphocyte builds up in the skin and start to attack the healthy skin cells by mistake. These T lymphocytes and the chemicals they produce trigger the skin to produce new skin cells at a faster rate than normal. The skin cells are created and then die in the space of a few days, rather than the normal cycle of 28 days. The dead skin cells build up on the surface of the skin, leading to the thickening, shedding and scaling of the skin.
Psoriasis has a tendency to run in families. It is believed that one in three people with psoriasis has a close relative with the condition.
Other factors that may trigger and exacerbate a flare-up of psoriasis include:
- Infections – some bacterial or viral infections such as streptococcal throat infections, Candida albicans (thrush), viral upper respiratory infections and HIV
- Injuries or trauma to the skin – operations, bites, cuts and severe sunburn
- Certain medicines – e.g. lithium (bipolar disorder medicine), ibuprofen (anti-inflammatory medicine), beta-blockers (blood pressure medicine), and antimalarial medicines
- Stress and anxiety
- Heavy alcohol intake and smoking
Common types of psoriasis
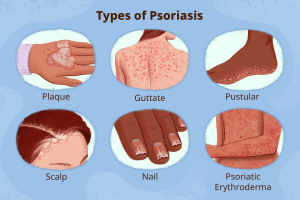
There are many different types of psoriasis. Usually, only one type appears at a time. Sometimes, two different types can occur together. One type of psoriasis may change into another type or may become more severe. Psoriasis appears in a variety of forms with distinct characteristics:
- Plaque psoriasis (psoriasis vulgaris) – the most common form of psoriasis, characterised by raised, inflamed, red lesions covered by a silvery white scale which can be itchy and sore. It can appear anywhere on the body, but is typically found on the elbows, knees, scalp and lower back.
- Guttate psoriasis – often starts in childhood or young adulthood after a streptococcal throat infection, characterised by small, red, individual spots on the skin. It usually appears on the trunk and limbs and often comes on quite suddenly. There is a chance that this type of psoriasis will disappear completely, or it can go on to develop plaque psoriasis.
- Flexural (Inverse) psoriasis – affects areas of the skin that are in folds or creases, such as the armpits, under the breasts, groin and between the buttocks. It appears as bright-red lesions that are smooth and shiny. It is made worse by rubbing and sweating because of its location in skin folds and tender areas, so it can be particularly uncomfortable in hot weather.
- Scalp psoriasis – occurs on parts of or the whole of the scalp, characterised by red patches of skin covered in thick silvery-white scales that can be extremely itchy, or have no discomfort at all. It can also cause temporary hair loss.
- Nail psoriasis – affects the nails, causing them to develop tiny dents or pits, become discoloured, loose, even crumble or separate from the nail bed.
- Pustular psoriasis – a rare type of psoriasis that causes pus-filled blisters (pustules) to appear on the skin. It can affect certain areas of the body, such as the hands and feet (palmo-plantar pustular psoriasis), or cover most of the body (generalised pustular psoriasis). It begins with the reddening of the skin followed by formation of pustules. The pus consists of white blood cells and is not infected. Generalised pustular psoriasis can be a medical emergency due to great inflammation.
- Erythrodermic psoriasis – a rare type of psoriasis that often affects most of the skin on the body, characterised by periodic and widespread fiery redness and intense itching of the skin, and the shedding of scales in sheets, rather than smaller flakes. It may occur in association with generalised pustular psoriasis. This type of psoriasis can cause the body to lose proteins and fluid and lead to serious illnesses such as infection, dehydration, heart failure, hypothermia and malnutrition, which often require hospitalization. Known triggers of erythrodermic psoriasis include the abrupt withdrawal of a systemic psoriasis treatment including cortisone; severe sunburns; infection; medications such as lithium, anti-malarial drugs; and strong coal tar products.
- Psoriatic Arthritis – about 30 percent of people with psoriasis also develop psoriatic arthritis (with or without skin lesions), which causes pain, stiffness and swelling in and around the joints. Some joints are particularly apt to be involved, including the last joint in the fingers or toes, wrists, knees, ankles or sacrum (lower back).
How TCM may help
 The condition that is congruent with psoriasis in Traditional Chinese Medicine is called “Niupixuan” or “Baibi”. According to TCM, Niupixuan is considered to be caused by an excess of “heat” in the skin which can manifest in different types such as blood-dryness, heat in the blood, blood stasis, damp-heat, or fire and toxic-heat. The “heat” often results from pathogenic wind entering the body and invading the Yin and blood. Also, Qi (vital energy) and blood stagnation throughout the body due to stress or emotional upset can result in heat accumulation. Niupixuan may also be caused by liver and kidney weakness as well as disharmony between the Penetrating (Chong) and Conception (Ren) vessels, between the Qi and the blood or between the Yin and Yang in the Zangfu.
The condition that is congruent with psoriasis in Traditional Chinese Medicine is called “Niupixuan” or “Baibi”. According to TCM, Niupixuan is considered to be caused by an excess of “heat” in the skin which can manifest in different types such as blood-dryness, heat in the blood, blood stasis, damp-heat, or fire and toxic-heat. The “heat” often results from pathogenic wind entering the body and invading the Yin and blood. Also, Qi (vital energy) and blood stagnation throughout the body due to stress or emotional upset can result in heat accumulation. Niupixuan may also be caused by liver and kidney weakness as well as disharmony between the Penetrating (Chong) and Conception (Ren) vessels, between the Qi and the blood or between the Yin and Yang in the Zangfu.
The TCM approach to psoriasis is to differentiate the syndrome and decide on what the underlying cause is. The aim of TCM treatment is to result in a permanent solution after treating the root cause of the illness.
Treatment should be based on the proper TCM check-up of the patient’s skin lesions, colour, shape, as well as symptoms, tongue and pulse. There are numerous TCM patterns associated with the various forms of psoriasis. The most common patterns seen include the wind-heat type, the blood dryness type, the blood stasis type, the toxic heat and dampness type and the excessive fire-toxin type. To clear the blood of its ailment, different combinations of Chinese herbs are prescribed, along with lifestyle modifications.
Chinese herbs are most commonly used for the treatment of psoriasis. They are used to help in restoring the balanced state of the body to allow psoriasis to be resolved. They are proven to have the following beneficial effects:
- Clearing pathogenic heat, cooling the blood, dispelling pathogenic wind and resolving toxins
- Nourishing blood and moistening dryness
- Promoting blood circulation and eliminating blood stasis
- Regulating the Chong & Ren vessels, balancing the Qi and blood as well as the body’s Yin and Yang
How we can help
In our clinic, Dr. Jim Xing has assisted many patients with psoriasis. acupuncture in Melbourne is his first treatment of choice but quite commonly he will also recommend acupuncture once a week. In all cases, he gives patients advice regarding their lifestyle, diet and supplement intake.
Looking for acupuncture eastern suburbs Melbourne? We offers acupuncture for eczema in Melbourne, acupuncture for migraine, and IVF acupuncture in Melbourne.
Book your appointment today
We are dedicated to helping you achieve the health and wellness that you desire. If you are interested, feel free to call us at our Frankston clinic on 9785 6688, or our Murrumbeena clinic on 9041 8879 to book an appointment today.

